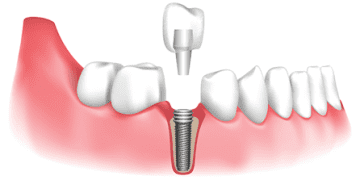
Mesothelioma is a rare industrial disease caused mainly due to asbestos exposure. A tumor starts growing in the protective lining of the lungs, abdomen, or in rare cases, the heart. Eventually, it starts to spread to other parts of the body. Unfortunately, mesothelioma can go undetected for decades and only starts showing concerning symptoms during the final stages of cancer. This accounts for the poor prognosis of this disease. Studies show that patients generally survive for 12 to 24 months after the Mesothelioma Prevalence diagnosis.
Table of Contents
How Common is Mesothelioma Prevalence?
Even though Mesothelioma Prevalence is deadly, few people suffer from it. According to a study, mesothelioma diagnosis makes up about 0.3% of all cancer diagnoses. That means roughly 3000 Americans are diagnosed with mesothelioma every year.
How Can it be Cured?
Mesothelioma is incurable. There is no cure for this deadly disease yet. Nevertheless, many therapeutic techniques increase the survival rate significantly. Most commonly, oncologists suggest surgery, chemotherapy, and radiation. Combined with traditional treatment, patients are also advised to go for alternative treatments to improve their prognosis. These treatments include immunotherapy and meditation, among others.
What Causes Mesothelioma Prevalence?
One of the major causes of mesothelioma is asbestos exposure. Asbestos is a fibrous mineral that is durable and fireproof. During the 1900s, asbestos was excessively used in construction. Even the US navy had ships that were constructed entirely of this material. It was only until the dangers became known that the use of asbestos became regulated.
Contrary to popular belief, asbestos is not the only causative agent of mesothelioma. Other factors like gender and genetics play a decisive role in the prevalence of this disease. This article will shed some light on how gender and genetics aid mesothelioma prevalence.
Gender and Mesothelioma
Men are most likely to suffer from mesothelioma than women. According to a study, 75% of the total mesothelioma patients are men. Women who suffer from mesothelioma generally have a better prognosis than men.
Why is that?
Men are usually exposed to asbestos directly. The most affected individuals are the ones who worked in construction and the US army between the 1930s and 1980s. Since these career paths are male-dominated, the ratio of male mesothelioma patients is significantly higher.
Although most women are not directly exposed to asbestos, they still make up 25% of the total mesothelioma patients. This happens due to secondary asbestos exposure. Secondary exposure, or second-hand exposure, happens when you come into contact with people who are directly exposed to asbestos. These people are usually family members who work in construction or the army. They bring asbestos fibers home, stuck to their clothing, hair, shoes, exposing people around them.
Overall, women have low asbestos exposure. In many cases, such exposure proves to be harmless. This makes them less likely to get diagnosed with mesothelioma at any stage of their lives.
What do the statistics say?
According to a study conducted in 2014, 13.4% of the women have a survival rate of 5 years after treatment. In contrast, only 4.5% of the men make it to 5 years.
Which type of mesothelioma occurs commonly in women?
According to research, more women are diagnosed with peritoneal mesothelioma. In contrast, men are more likely to be diagnosed with pleural mesothelioma.
Peritoneal mesothelioma is more survivable than pleural mesothelioma. The credit for this goes to a technique called Heated Intraperitoneal Chemotherapy (HEPEC). This therapy combines surgery with chemotherapy to treat peritoneal mesothelioma and increases the survival rate of patients by a few years. A study was conducted in 2018 regarding the success rate of HEPEC. Around 75 peritoneal mesothelioma patients were treated with HEPEC, and their survival rates were increased by eight years. 45% of these patients were women.
Genetics and Mesothelioma
Not everyone who is exposed to asbestos gets diagnosed with mesothelioma. However, there are some families reported to have multiple mesothelioma patients in their family. This proves that some people readily succumb to asbestos poisoning compared to others.
Scientists found out that the problem lies with a gene responsible for making a protein named BAP1. It is a tumor suppressor gene present in the genetic code of all human beings. The main role of this gene is to identify tumor formation in the body and suppress its growth.
Sometimes, the BAP1 gene is found to be mutated. This mutation makes the identification and suppression of a tumor much difficult. A mutated BAP1 gene can mask mesothelioma from the body’s immune system for a long time. In 2011, a study was conducted to prove the involvement of the BAP1 gene in mesothelioma.
Genetic Risk Factors
Although there is not much you can do to fix a genetic mutation, you can be prepared ahead of time and take necessary precautions. You can have a mutated BAP1 gene due to the following factors:
- Excessive Asbestos Exposure: Long-term exposure to asbestos can alter your normal BAP1 gene. Asbestos fibers can mutate a perfectly healthy BAP1 gene to form tumor cells and go undetected.
- Hereditary: In some families, a mutated BAP1 gene is inherited. Even if you have never been exposed to asbestos, you may have a mutation in the BAP1 gene, putting you at high risk for mesothelioma.
Using Genetics to our Advantage
Once the mutation in the gene was discovered, a study was published in 2017 that proved that low levels of BAP1 can make mesothelioma patients less responsive to chemotherapy. This was because BAP1 is involved in DNA repair.
The researchers proposed that if levels of BAP1 are restored before administering chemotherapy, patients have a good chance to respond well to the treatments.
Wrap-up
There is no safe limit for asbestos exposure. Patients who are diagnosed with mesothelioma have no idea when and how they got exposed. It is important to take precautionary measures, especially if you work in an asbestos-rich environment.
Wear protective clothing and keep your work clothes separate from your home clothes. Schedule a regular screening without waiting for warning symptoms. Remember, it is better to be safe than sorry!